Every year on 26th September, the world celebrates World Contraception Day (WCD), a day initiated by NGOs to raise awareness about contraception. The global campaign is aimed at helping couples make informed decisions about their sexual and reproductive health, so that every pregnancy is wanted.
In a study by the National Population and Family Development Board (NPFDB), only 52.2% of married Malaysian women (aged 15 to 49) use family planning methods, a low figure compared to our other Asian counterparts. The lack of contraceptive uptake is mainly due to difficulty gaining spousal consent and misconceptions about contraceptive side effects.
What are my options?
You might be surprised at the choices when it comes to birth control. Contraceptives can be short-acting, long-acting, one-time, and sometimes permanent, with most methods made for women. Despite the abundance of choices available, the highest methods used by adults in Malaysia are condoms and pills – at 81.7% and 60.8% respectively.
Contraception is more than just condoms and pills, though. According to the Ministry Of Health (MOH), contraceptive methods are classified into two major groups: non-hormonal and hormonal.
Non-hormonal Contraceptive Methods
Non-hormonal contraceptives consist of no products (natural method) or physical products (barrier method). Breastfeeding mothers who have issues with their milk supply and women who have concerns about the side effects of hormonal birth control can opt for these as an alternative.
Natural Method

Photo credit: theAsianparent
1. Fertility Awareness-Based (FAB) Method
This method involves a woman charting her menstrual cycle, taking her basal body temperature, and observing her cervical mucus or vaginal discharge to identify fertility signs and track ovulation. It is a form of natural family planning where couples avoid intercourse or resort to other birth control methods on days leading to ovulation.
- Pros: No physical or chemical products are used
- Cons: Does not protect against STIs. Factors such as medication, illness and stress can disrupt fertility signals
- Typical use effectiveness: 12-24 pregnancies per 100 women per year, depending on methods used
2. Lactation Amenorrhoea Method (LAM)
Women who do not have their periods while breastfeeding can use the Lactation Amenorrhoea Method (LAM) as a temporary form of birth control. Breastfeeding women produce less oestrogen due to the increased levels of prolactin which prevents ovulation. LAM is ideal for the first six months after childbirth, upon condition that the woman hasn’t resumed her menstruation and the baby is fully or nearly fully breastfed with very little to no formula.
- Pros: Begins immediately postpartum and does not interfere with sexual intercourse, as no external method is used
- Cons: Only a temporary method of contraception and the baby should be breastfed exclusively for 6 months, which may be difficult for some. Certain medications may also interfere with effectiveness of LAM
- Typical use effectiveness: 2 pregnancies per 100 women in 6 months
3. Withdrawal (or “pulling-out”) Method
The withdrawal method keeps sperm away from the vagina by “pulling out” the penis before ejaculation. It requires timely, self-controlled withdrawal by the male and is not as effective as other methods, given that even a tiny amount of semen can cause pregnancies. Even if done correctly, there might be semen in pre-ejaculation (or ‘pre-cum’), an involuntary fluid released right before ejaculation.
- Pros: No side effects and can be used when no other contraceptives are available
- Cons: Does not protect against STIs and may be difficult to pull out in time
- Typical use effectiveness: 20 pregnancies per 100 women per year
Barrier Method

Photo credit: Malay Mail
1. Male (External) Condoms
A condom is a thin tube worn and fitted over an erect penis, and is one of the most commonly used barrier methods. Most condoms are made of latex, but there are also condoms made of Polyurethane for those with latex sensitivity. Only use a condom once, and never reuse one, even if the male did not ejaculate.
- Pros: Easily obtained and reduces the risk of STIs
- Cons: A condom may split or tear if not used properly and may not suitable for those allergic to latex, plastic or spermicides
- Typical use effectiveness: 13 pregnancies per 100 women per year

Photo Credit: Contraception Choices
2. Diaphragm
A diaphragm is a small, cup-shaped disc that covers the bottom of the cervix. For higher effectiveness, use diaphragms with spermicide, which is a chemical that kills sperm. Diaphragms can be placed in the vagina an hour before intercourse and should remain for 6 hours up to 24 hours.
- Pros: Small and reusable. Fertility can be regained immediately upon removal
- Cons: Does not protect against STIs and not suitable for women who are sensitive to latex, silicone or spermicides. There is also a possibility of the diaphragm dislodging during intercourse
- Typical use effectiveness: 17 pregnancies per 100 women per year

Photo Credit: Mayo Clinic
3. Cervical Cap
A cervical cap is a cup made of reusable silicone or latex, and should be used with spermicide. Unlike diaphragms, cervical caps are fitted tightly on the cervix itself. It can be inserted hours before intercourse and used for up to 48 hours.
- Pros: Small and reusable. Fertility can be regained immediately upon removal
- Cons: Does not protect against STIs, and not suitable for women who are sensitive to latex, silicone or spermicides. There is also a possibility of the cervical cap dislodging during intercourse
- Typical use effectiveness: 32 pregnancies per 100 women who have given birth per year, and 16 pregnancies per 100 women who have not given birth per year
Hormonal Contraceptive Methods
Hormonal contraceptive contains a combination of progestin and oestrogen or progestin alone, which suppresses ovulation, thickens the cervical mucus, and thins the uterus lining. This makes it difficult for fertilization, implantation and the releasing of an egg to occur. Contraception options include injections, pills, implants, or intrauterine devices (IUD).

Photo Credit: How You Know
1. Combined Oral Contraceptives (COCs) or ‘The Pill’
There are two types of contraceptive pills: combined oral contraceptives (COCs, or ‘the pill’) and progestin-only pills (POPs or ‘the mini pill’). COCs consist of both oestrogen and progestin that prevent pregnancy. These pills may come in several forms, depending on the brands and types you choose.
- Pros: May help reduce acne, and the risk of fibroids, ovarian cysts, non-cancerous breast disease, cancer of the ovaries, womb and colon
- Cons: Does not protect against STIs and must be taken around the same time every day for it to be effective. Some medications may interfere with its effectiveness and may increase blood pressure
- Typical use effectiveness: 7 pregnancies per 100 women per year
2. Progestin-only Pills (POPs) or “The Mini pill”
Single hormone pills are suitable for women who cannot tolerate oestrogen-based contraception, such as the COC pills and patches. These pills are available in two forms: 3-hour progestin-only pills and 12-hour progestin-only pills.
- Pros: Does not affect breastfeeding
- Cons: Does not protect against STIs and must be taken around the same time every day for it to be effective. Some medications may interfere with its effectiveness
- Typical use effectiveness: 7 pregnancies per 100 women per year

Photo Credit: Obgyn
3. Implants
A contraceptive implant is a small flexible plastic rod, almost the size of a matchstick implanted under the skin of your upper arm. The procedure is painless and typically feels like an injection. An implant can remain in the body for three years, providing long-term protection against pregnancy. Just like the progestin-only pills, implants are practical for those who can’t use oestrogen-based contraception.
- Pros: Safe for breastfeeding. Fuss-free and there is no daily action required unlike oral contraceptives
- Cons: Does not protect against STIs. May cause irregular bleeding, lighter periods or no periods at all. Side effects may possibly include weight gain, nausea, breast and abdominal pain
- Typical use effectiveness: 0.1 pregnancies per 100 women per year

Photo Credit: Hello Doktor
4. Injection
A birth control injection works by releasing the hormone progestin into the body, preventing pregnancies. It requires regular visits to the doctor, typically every three months. If you decide to go off the injection, it may take between 12-14 weeks to regain fertility, and up to a year to conceive.
- Pros: Safe for breastfeeding. Fuss-free and there is no daily action required unlike oral contraceptives
- Cons: Injections must be taken on time for it to work. Depending on the individual, there may be some side effects such as weight gain, mood swings, and changes to your menstruation
- Typical use effectiveness: 4 pregnancies per 100 women per year

Photo Credit: Hello Doktor
5. Patch
A contraceptive patch is a thin patch that is stuck anywhere on your skin (except breasts). It releases the same hormones and works in the same way as the combined pills. A patch is used and changed weekly for three weeks, with no patch being worn on the 4th week to trigger menstruation.
- Pros: More convenient than pills as patch only needs to be changed weekly
- Cons: Doesn’t protect against STIs. The patch may be visible and cause skin irritation. Temporary side effects may occur (such as mood swings, nausea, headaches), but will subside after a few months
- Typical use effectiveness: 7 pregnancies per 100 women per year

Photo Credit: MPR
6. Hormonal Intrauterine Device (IUD)
An Intrauterine Device (IUD) is a tiny T-shaped device inserted into the uterus and remains inside for 3-5 years. There are two types of IUDs; hormonal and non-hormonal (copper). Slow-releasing hormone progestin in hormonal IUDs makes it one of the most effective forms of contraception.
- Pros: Highly effective and provides long-term protection of up to five years. It may also help reduce menstrual pain and lessen bleeding
- Cons: Doesn’t protect against STIs. There is also a rare risk of the IUD slipping out of place
- Typical use effectiveness: 0.7 pregnancies per 100 women per year
Sterilisation
Sterilisation is a form of contraceptive which involves surgery for couples who desire a more permanent approach. Reversal can be difficult and is an option for those sure they do not want more children or any children.

Photo Credit: Parents
1. Tubal Ligation (Female)
You may have heard of women who have had their “tubes tied” as a way to prevent pregnancy. This procedure is called tubal ligation, a form of female sterilisation where surgery is performed on the fallopian tubes and “tied” so that eggs have no chance of being fertilised. Female sterilisation can be done at any time, even immediately post-delivery. There are some risks that one should consider, such as the rare possibility of the fallopian tubes growing back together, making the female fertile again.
- Pros: Highly effective and does not affect your hormone levels nor menstruation
- Cons: Does not protect against STIs and as with any surgery, there may be minor complications such as infection and internal bleeding
- Typical use effectiveness: 0.5 pregnancies per 100 women per year
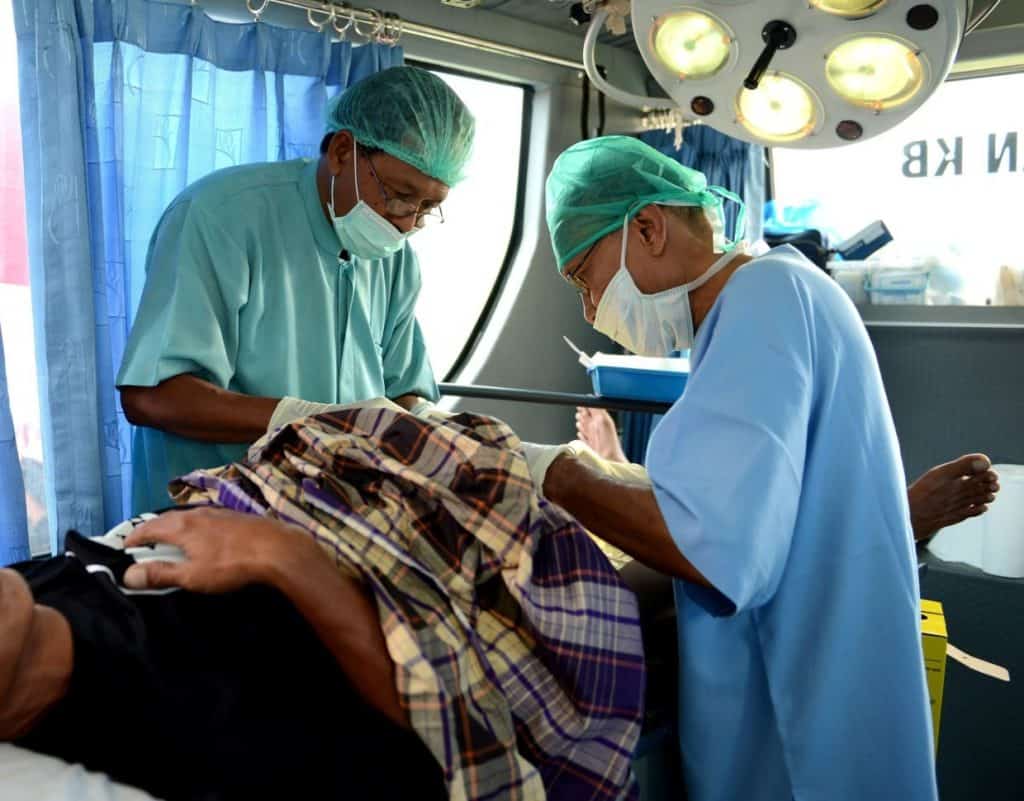
Photo Credit: The Star
2. Vasectomy (Male)
Besides condoms, the other contraception available for males is a vasectomy. This form of sterilisation is a surgery that cuts or blocks the tubes in the scrotum, stopping sperm from reaching the semen during ejaculation. A vasectomy has lower risks and is a less complicated procedure compared to female sterilisation. As with tubal ligation, there is also a rare possibility of the tubes reattaching, causing pregnancy.
- Pros: Highly effective and does not affect your testosterone levels
- Cons: Does not protect against STIs. Vasectomies do not work immediately, and follow-ups are crucial to ensure there are no more sperm in the semen
- Typical use effectiveness: 0.1 pregnancies per 100 women per year
Emergency methods
Should you engage in unprotected sex or experience contraceptive failures, emergency contraception may help. These methods only work within a small timeframe, but are more effective when done soon after intercourse.

Photo Credit: NHS
1. Emergency Contraceptive Pills (ECP)
Most people call it the “morning-after pill” but contrary to its name, these pills are best taken immediately, preferably within 72 hours, or up to 120 hours, after unprotected sex. Two types work to delay or prevent the release of eggs from ovaries: Levonorgestrel (e.g. Postinor-2 or Escapelle) and Ulipristal (e.g. Ella).
- Pros: Can be easily obtained from local pharmacies
- Cons: There may be unwanted side effects from changes to your menstruation to nausea and abdominal pain. It does not protect against STIs and needs to be taken within a limited time frame
- Typical use effectiveness: Less than 1 pregnancy for progestin-only ECP and 2 pregnancies for combination of oestrogen and progestin per 100 women per year

Photo Credit: Unsplash
2. Copper Intrauterine Contraceptive Device (IUCD)
Though considered an emergency option, the copper IUCD may also provide a long-term contraception solution. It is best to insert the IUCD within five days of unprotected sex which will immediately work to prevent implantation. Once inserted, the IUCD can remain inside until the next menstruation or the next 3 to 5 years.
- Pros: Copper IUCDs are non-hormonal and safe for breastfeeding. Once inserted, they work immediately to provide long-term prevention
- Cons: Does not protect against STIs and some people may experience heavier periods. There is also a rare risk of the IUD slipping out of place
- Typical use effectiveness: 0.8 pregnancies per 100 women per year
Contraceptive services are commonly available at both private and public health facilities. For those looking at affordable options, Klinik Nur Sejahtera LPPKN provides family planning services at a small fee. You can even purchase certain types of contraceptives without a prescription at your local pharmacies.
DOC2US‘ telepharmacy platform also helps to educate women about their reproductive health and empower them to make informed family planning decisions through accessible oral contraceptive and free teleconsultation by pharmacists.
You could also try ‘Ask Maya’, Bayer Malaysia’s very own chatbot dedicated to family planning.
When it comes to family planning, there isn’t a one-size-fits-all option. It may take several tries before you can decide on a method that works comfortably for both you and your partner. Choosing a contraception method is a personal right, so have an open discussion with your healthcare provider on the options that best suit your needs, budget, lifestyle, and overall health.










